
In fetuses with bradycardia, a slow ventricular escape rate of less than 55 beats/minute appears to be poor prognostic factor. 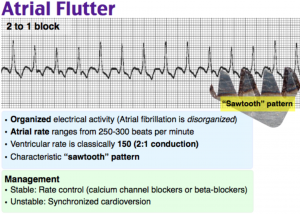
Earlier onset in gestation of a tachyarrhythmia and a higher ventricular rate are other risk factors associated with a greater risk for development of hydrops fetalis. Hence, patients with hydrops and a normal heart rate warrant repeat assessment of the fetal heart rate to detect intermittent arrhythmias. Intermittent tachycardias can also be associated with hydrops. If the arrhythmia is sustained, there is a greater risk of fetal hemodynamic compromise leading to hydrops fetalis and fetal demise. įetal arrhythmias are usually detected during routine auscultation of the fetal heart or during an obstetric scan. In approximately 10% of pregnancies complicated by fetal arrhythmias, the arrhythmia may be life-threatening. Fetal arrhythmias can be detected in approximately 1% of all fetuses and up to 49% of all referrals for fetal echocardiography. Other arrhythmias include tachyarrhythmias (heart rate in excess of 160 beats/min) such as atrioventricular (AV) reentry tachycardia, atrial flutter, and ventricular tachycardia, and bradyarrhythmias (heart rate <110 beats/min) such as sinus node dysfunction, complete heart block (CHB) and long QT syndrome (which is associated with sinus bradycardia and pseudo-heart block). Most of the fetal rhythm disturbances are the result of premature atrial contractions (PACs) and are of little clinical significance. The rate, duration, and origin of the rhythm and degree of irregularity usually determine the potential for hemodynamic consequences. A fetal heart rate is considered abnormal if the heart rate is beyond the normal ranges or the rhythm is irregular. Arrhythmias that are drug-refractory or poorly tolerated have been treated with catheter ablations during pregnancy in experienced centers with techniques to reduce fluoroscopic exposure.The normal fetal heart rate ranges between 110 and 160 beats per minute. Catheter ablation procedures are generally avoided during pregnancy.Amiodarone should be avoided if possible. Quinidine therapy should be managed by an experienced electrophysiologist. Quinidine, procainamide, lidocaine, flecainide, propafenone, and sotalol cross the placenta but do not have known teratogenic effects and can be used during pregnancy.Verapamil is preferred over diltiazem during pregnancy, and both are compatible with lactation. Calcium channel blockers are considered second-line agents.Beta-blockers are compatible with lactation. Neonatal hypoglycemia and bradycardia are rare possibilities. There is a small risk of fetal growth restriction with long-term treatment, but no increased risk of congenital malformations. Beta-blockers can be used during pregnancy.Preparation should be made for emergency cesarean delivery. Manual lateral displacement of the uterus can improve venous return and cardiac output. Medication doses and defibrillation protocols are unchanged. Cardiac arrest should be treated the same as for non-pregnant patients.In the absence of structural heart disease, beta-blockers and antiarrhythmic medications such as flecainide and sotalol can be used safely during pregnancy to treat tachyarrhythmias.Atrioventricular nodal blocking agents can increase conduction over the accessory pathway and may degenerate to ventricular arrhythmias. Patients with evidence of pre-excitation should be treated with caution.Long-term suppression can be achieved with beta-blocker therapy (first-line), or digoxin or calcium channel blockers as second-line therapy. Supraventricular tachycardia can be treated acutely with vagal maneuvers and adenosine.Normal heart rate progressively increases during pregnancy by 10-25% from pre-pregnancy values.Proarrhythmic mechanisms may include increased plasma catecholamine concentrations, chronotropic effects of relaxin, mechanical effects of atrial stretch, increased ventricular end-diastolic volume due to volume expansion, and hormonal changes. Benign premature atrial and ventricular contractions are common. Pregnancy is associated with increased incidence of arrhythmias.The following are key points to remember from this state-of-the-art review of arrhythmias in pregnancy:
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
